In August 2019, Vodafone partnered with the ASSERT centre (Application of the Science of Simulation to Education, Research and Medical Technology) in University College Cork, Ireland, to create the first 5G connected telemedicine and medical robotics training centre in the world. Its aim is to provide a test-bed facility for the MedTech sector, preparing devices for the roll-out of 5G
Here, Professor Barry O’Reilly, Director of ASSERT, discusses some of the innovations happening at ASSERT and the impact 5G could have on the evolution of healthcare.

Anne O’Leary, Vodafone Ireland CEO, and Professor Barry O’Reilly
Professor Barry O’Reilly, a specialist consultant in obstetrics and gynaecology, is passionate about technology and its role in driving innovation in healthcare. He believes that Covid-19 has become a catalyst for change in the industry, sparking new ideas and encouraging medical professionals to embrace new ways of working.
“There has been a longstanding reluctance among health professionals to embrace digital technology and change traditional clinical management, particularly if it has been standard practice for a long time,” he says. “The pandemic put us in a position where we all had to think differently.”
At the beginning of the pandemic, healthcare workers were among those most affected by and at risk from the virus. In January 2021,when Ireland was experiencing its third wave – 65% of Covid-19 patients had caught the virus in a hospital. To help keep their wards safe, Barry and his colleagues worked with a local software development company (8 West) to develop a Covid-19 remote early warning system (CREW), which utilised wearable devices to monitor temperature, heart rate and other parameters that would indicate the wearer was becoming unwell and should self-isolate.
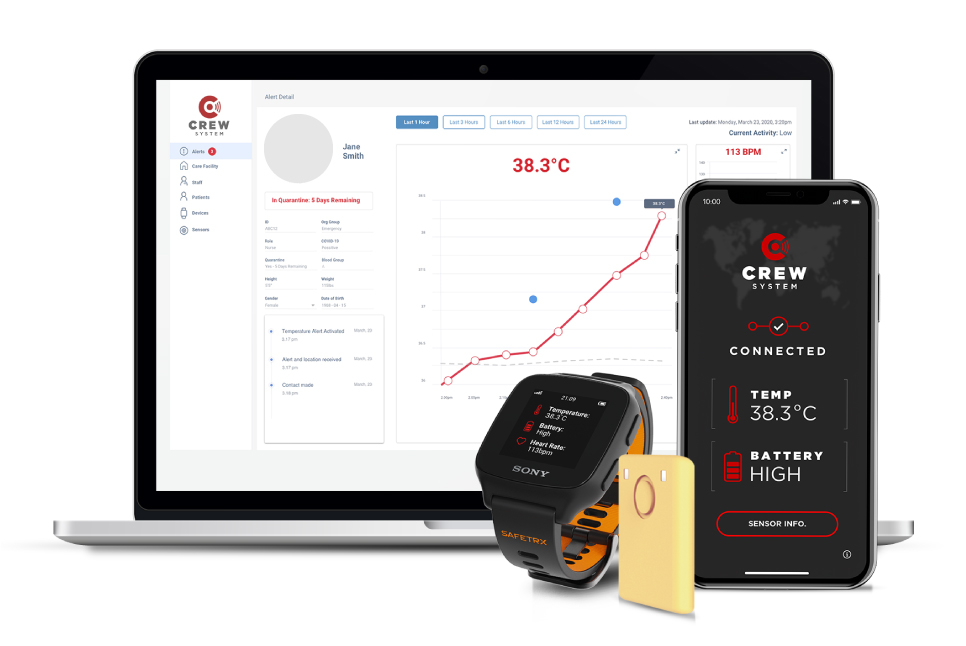
ASSERT and 8 West created the Covid-19 remote early warning system (CREW)
This was a small but useful step in helping limit the spread of infection, particularly when regular Covid-19 testing wasn’t as easy to access as it is today. Barry and his team are already applying the lessons learned from this to other scenarios, where it could be more beneficial for the monitoring of patients to take place remotely, rather than having those patients attend overcrowded waiting rooms.
Enabling access to global healthcare services
Barry has always held an interest in the way robotics can be used to improve the safety and success rates of surgical procedures. In 2007, Barry became the first surgeon in the British Isles to use a robot to conduct a hysterectomy. Now, at the ASSERT centre, he is exploring how 5G can improve robotic surgery by enabling it to be conducted remotely, eliminating lag time between the surgeon console and the surgical instruments (i.e. between the surgeons and their patients).
This could open new possibilities for the healthcare sector, enabling patients all over the world to access medical expertise that may not be available to them right now.
“Imagine a child in Ireland who has developed a very rare type of cancerous tumour,” says Professor O’Reilly. “Removing that tumour might require complex surgery that may only be available in a few centres in the world. Often what happens is the family of the child needs to fundraise to pay for the child to travel to these select centres, such as Memorial Sloan Kettering Cancer Centre in the USA, have the operation and then stay in accommodation to recover for the next few weeks before returning home to Ireland.
“Remote surgery could have a transformative impact in situations like this. A surgeon in America could perform an operation in Ireland, using robotics. The biggest challenge we face in making that a reality is the lag time or patchy connectivity. Seconds count in surgery – urgency is key. But the speed and stability of 5G could solve that problem.”
Transforming medical training
5G connectivity and emerging technologies are also having an impact on the world of medical training.
“The future of medical training is digital, especially in a world where surgery could soon be conducted through digital means,” says Professor O’Reilly.
ASSERT is working with companies like REACTS in Canada whichhave developed a platform to enable remote ultrasound and surgical training over a video link. Cameras are set up in surgical theatres to film and transmit live video of an operation, allowing medical trainers to supervise and instruct their students. 5G connectivity could enable this to happen in real time, regardless of the distance between them. The platform also allows trainers to use augmented reality to overlay 3D images, such as anatomical diagrams, on live streams.
And emerging technologies, such as artificial intelligence (AI), could help take digital training to the next level. For example, AI models could be used in training and exams to analyse and measure performance – how a student is moving a particular instrument, how long they are taking, how effective their technique is, and so on. This could help examiners avoid subjective judgement in their marking.
But the most exciting part about the role of 5G and technology in healthcare? The best innovations are yet to come.

























